Homepage // Blog / Our Favorite Combination Treatments
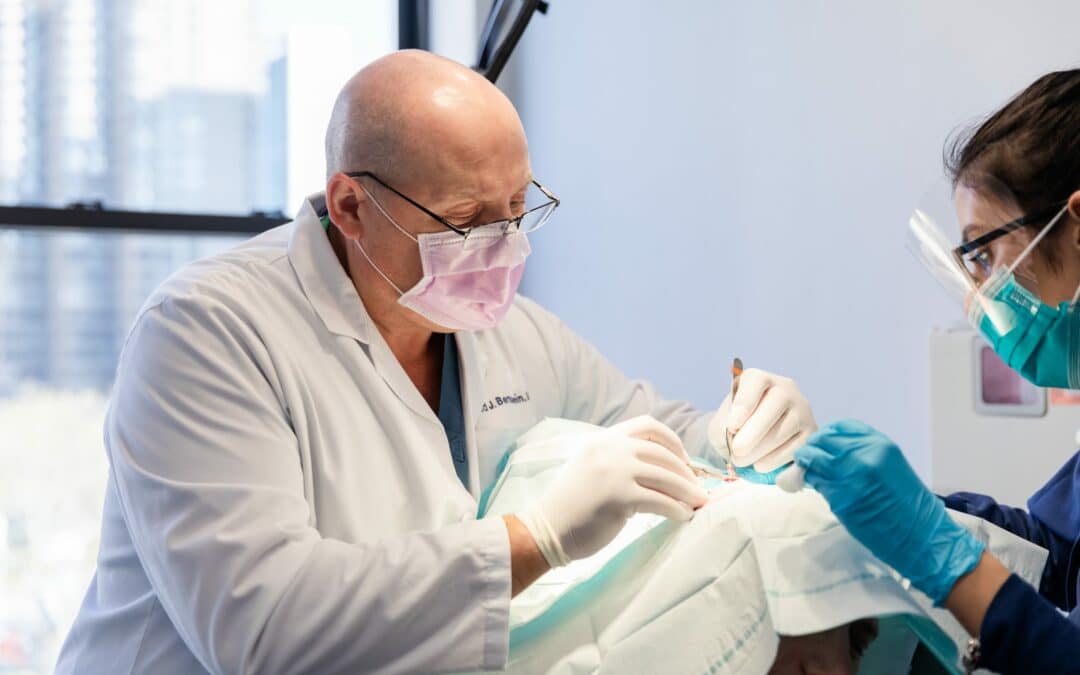
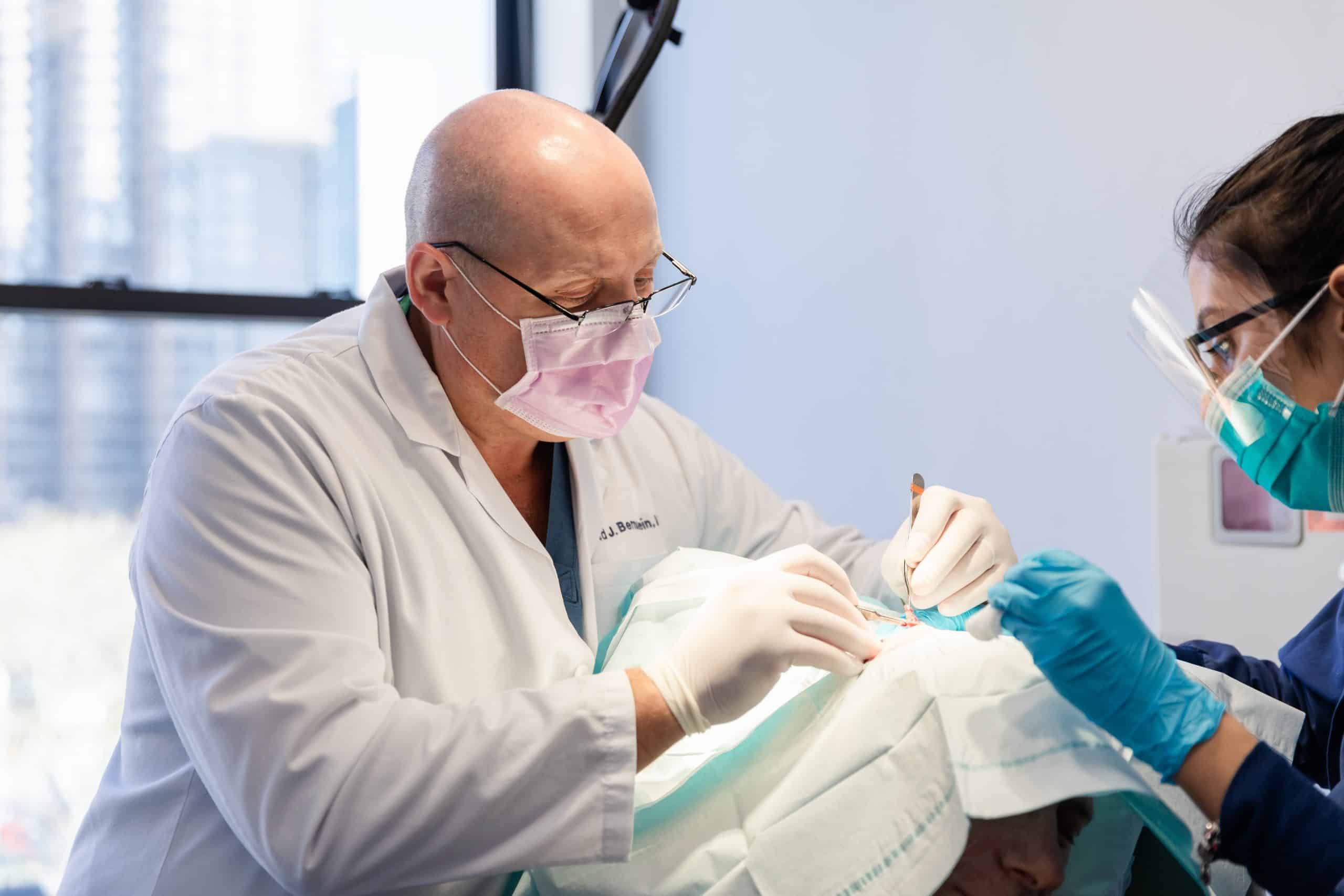
Skin Cancer Screening, Treatment & Mohs Surgery
When detected early and treated promptly, most skin cancers are curable. Our board-certified dermatologists have extensive experience in diagnosing and treating skin cancer, and many have been fellowship trained in Mohs Surgery under Dr. Roy G. Geronemus. With our expertise and qualifications, you can rest assured that we will provide you with the most effective treatment options available in Manhattan and Southampton, New York.
At the Laser & Skin Surgery Center of New York, we believe screening exams and consults are the cornerstones of effective prevention strategies against skin cancers. However, the first step is educating yourself about the disease. One of our board-certified dermatologists and Mohs surgeons, Dr. Leonard Bernstein, conducted a webinar that focuses on the importance of skin cancer screening, prevention, and the available treatment options. Below, we share the highlights.
Skin Cancer Basics
In his webinar, Dr. Bernstein pointed out that skin cancer is the most common form of cancer in the United States, with more people diagnosed with it each year than all other cancers combined.
There are over 5 million non-melanoma skin cancer (NMSC) diagnoses in the US each year with approximately 2,000 deaths, and 20% of the population will develop NMSC by age 70. Organ transplant patients and connective tissue disease patients who are immuno-compromised due to medications are also far more likely to develop NMSC.
Melanoma skin cancer, on the other hand, accounts for 200,000 new diagnoses and 7000 deaths annually. Fortunately, half of the diagnoses are superficial as patients and doctors are identifying them sooner which prevents spread and improves the cure rate for these potentially deadly cancers.
To read more about the basics of skin cancer, please visit cdc.gov.
Who should get screened?
Dr. Bernstein says screenings are particularly critical for adults who:
- Are over 25 years of age
- Have a history of numerous sunburns or have frequently used tanning beds in the past
- Are immuno-suppressed
- Have a family history of melanoma
- Have a large number of irregularly shaped moles (those who have dysplastic nevus syndrome have increased risk for certain skin cancers)
- Have a history of skin cancer
Or for children who:
- Have a strong family history of melanoma
- Have dysplastic nevus syndrome
- Have a history of giant congenital nevus (moles that cover up large portions of the body
If you have lots of atypical moles, get your skin looked at twice a year. When you have melanomas, visit your dermatologist frequently in the first five years. This helps to identify abnormal growths in a timely manner as early identification and treatment prevent skin cancers from progressing and allow for curative treatment.

Screening For Skin Cancer
Dr. Bernstein recommends an appointment with a dermatologist for your skin check. Dermatologists are experts in all skin diseases. Mohs surgeons, specifically, are cutaneous oncologists who specialize in skin cancer and therapies.
Skin examinations are typically done in a dermatologist’s office, but telemedicine is also available. However, tele-consults are far inferior compared to a physical exam. Dermatologists need to be able to see and touch lesions in person and use magnifying devices (dermatoscopes) that help them look at subtle minute patterns in the lesions, helping them make a proper diagnosis. Essentially, a skin examination involves a systematic check of your skin from head to toe, covering every inch of the body.
Skin cancer screening may include:
Dermoscopy – This device looks more closely at the pigment patterns in the skin, helping dermatologists define whether a mole is abnormal or irregular.
Body Photography – Pictures are taken of patients who have abnormal-looking moles, which are observed over time to see if they’re changing. There are outside companies, such as MoleSafe, that do this professionally. Moles are cataloged through full-body imaging combined with dermoscopic technology, which allows dermatologists to track changes.
Biopsy – This procedure removes all or a portion of the lesion for microscopic exam.
Optical Coherence Tomography and Reflective Confocal Microscopy – These devices look through the skin like a microscope, allowing dermatologists to magnify and define lesions. They are also used to define tumor borders.
Learn Your ABCDEs
The ABCDEs of melanoma detection are:
- Asymmetry – one half of a lesion is not a mirror of the other half
- Border – the borders have an irregular shape or have scalloped edges
- Color – multiple colors are often mixed in an irregular fashion
- Diameter – greater than ¼ inch, 6 mm, or the size of a typical pencil eraser
- Evolving – a change in a previously stable mole
Essentially, the ABCDEs serve as a memory tool that summarizes the warning signs of skin cancer to keep in mind as you do your own skin checks at home. If you see any of these features, bring them to your dermatologist’s attention as soon as you spot them, so your doctor can assess them and determine whether further assessment is necessary.

Skin Cancer Prevention
The best thing you can do to prevent skin cancer is to protect your skin from the sun. Wear sunblock with at least SPF30 and preferably one that has both UVA and UVB protection. SPF is just a multiple of how long it takes for your skin to burn. For instance, if you normally become red after 10 mins in the sun without sunscreen, a SPF30 sunscreen will give you protection for approximately 30 times longer or 300 mins (5 hours).
What is the difference between sunscreen and sunblock?
Sunscreen consists of chemicals that need to interact with your skin 30 minutes prior to sun exposure. Active ingredients include avobenzone, PABA, octinoxate, oxybenzone, homosalate, octocrylene, ecamsule, and octisalate. Sunblocks, on the other hand, are mineral-based, typically consisting of zinc oxide and titanium dioxide, which are physical blockers that immediately block out the sun’s UV rays. As soon as you put them on, you have protection.
Recent FDA reports state that chemicals used in some sunscreens have been found to be elevated in the blood for days to weeks after regular use for a short period of time and in some cases, also harmful to aquatic life. The FDA is proposing that two ingredients are “generally recognized as safe and effective” (GRASE). These ingredients are titanium dioxide and zinc oxide.
UPF (ultraviolet protection factor) clothing may also be worn for sun protection. Solumbra, Coolibar, and Solbari are companies that produce clothing that protect you from the sun without having to put on sunblock underneath them.
What is Non-Melanoma Skin Cancer?
Non-melanoma skin cancer represents a group of cancers that gradually develop in the upper layers of the skin. The term “non-melanoma” distinguishes these more common types of skin cancer from the less common and more serious skin cancer known as melanoma.
Risk Factors:
- Excessive sun exposure over a lifetime
- Frequent sunburns, especially in youth
- History of radiation exposure
- History of arsenic exposure
- History of old scars
- History of “pre-skin cancer” (actinic keratosis)
- Past history of skin cancers
- Genetic disorders – xeroderma pigmentosum, basal cell nevus syndrome
- History of human papilloma virus (HPV)
- History of smoking
Skin cancer develops when skin cells that make up your skin reproduce abnormally in the epidermis, the skin’s outermost layer. They can mutate and metastasize, forming malignant tumors or spreading through other parts of the body.
Chronic sun damage can cause changes in the skin that can precede the development of skin cancer.
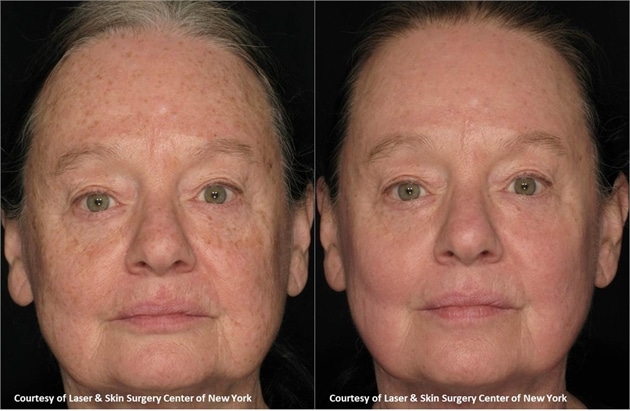
What is Actinic Keratoses?
- A type of pre-cancer
- Common growth seen in photodamaged skin as a direct result of excessive UV exposure
- Characterized by reddish, rough patches, bumps in the skin, or a slight brownish hue
- Often felt sooner than seen, and can occasionally be uncomfortable if rubbed or pressed
- Considered a precursor to squamous cell carcinoma (approximately 5-10% will evolve to SCC)
- Often seen in association or on the surface of SCC or basal cell carcinoma (BCC)
Learn more about actinic keratosis.
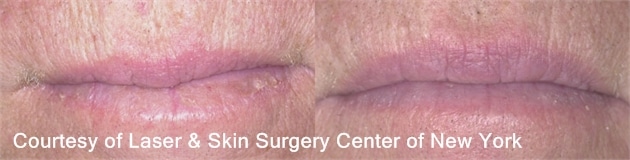
What is Actinic Cheilitis?
- actinic keratosis of the lip
- High risk of transformation into SCC
Learn more about actinic cheilitis.
Primary Types of Skin Cancer
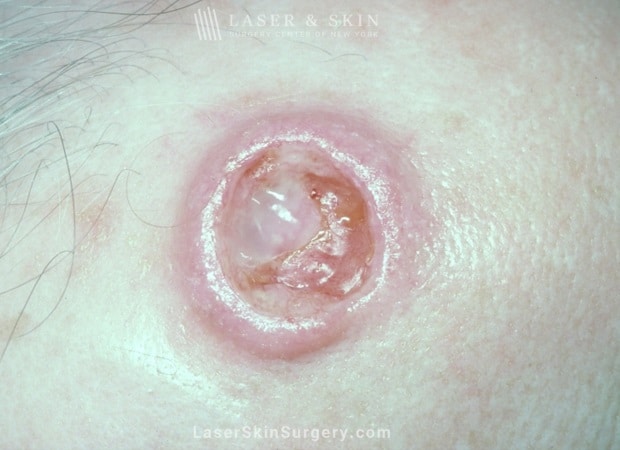
Basal Cell Carcinoma (BCC)
- Most common cutaneous malignancy
- 70-75% of NMSC are basal cell carcinoma
- Arises from uncontrolled growth of basal cells in the epidermis
- Clinical appearance includes pearly bumps, sores that don’t heal, red, rough skin, brown, scaly patches, ulcers, red bumps
- Slow growing in general
- May remain superficial or invade deep in the skin or underlying tissue (muscle and bone)
- Major risk factor is sun exposure
Learn more about basal cell carcinoma.
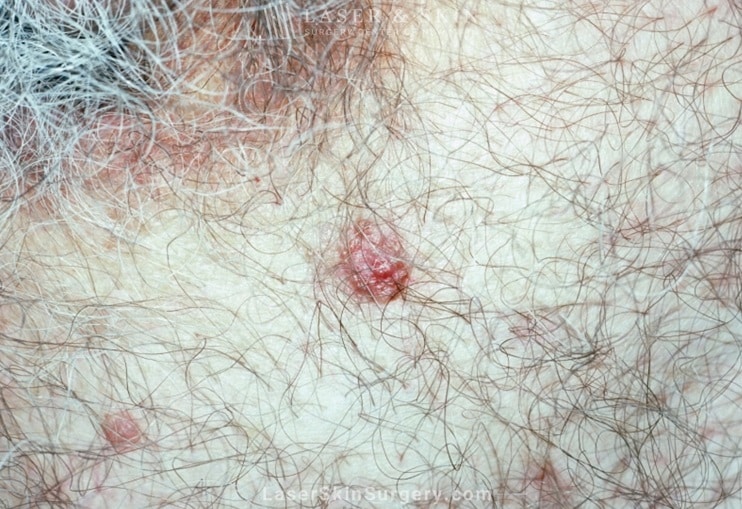
Squamous Cell Carcinoma (SCC)
- Second most common cutaneous malignancy
- 20% of NMSC are squamous cell carcinoma
- Arises from uncontrolled growth of mid-layers of the epidermis
- Clinical appearance includes red, rough patches, red bumps, ulcers, bumps with central craters
- Squamous cell carcinomas have a greater risk of distant spread than BCC
- Most common NMSC to develop in organ transplant patients and immune-compromised people
Learn more about squamous cell carcinoma.
Dermatofibrosarcoma Protuberans (DFSP)
- Very slow growing malignancy of cells in the mid-layer of the skin (dermis)
- Rarely spreads through the body but can grow deep and wide
- Clinical appearance includes red or brownish bump or “knot” in the skin
- May have a firmness of the skin well beyond the elevated portion
- Grows like an iceberg (the surface size is often much smaller than the deeper portion as it spreads easily in the fat layer, which is directly below the dermis
- Can affect all ages but most common in ages 20-50
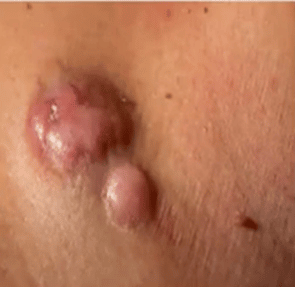
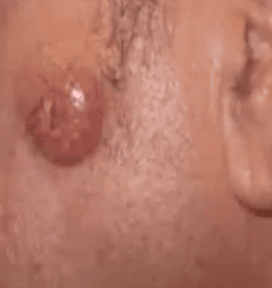
Merkel Cell Carcinoma
- A rare form of NMSC (3000 cases annually)
- Aggressive tumor with a high rate of spread (metastasis) and recurrence
- Clinical appearance includes pink to red bumps (nodules), can be ulcerated often on head or neck but can be seen elsewhere
- Risk factors are UV exposure, history of other NMSC or melanoma, mostly seen in men and people above age 50
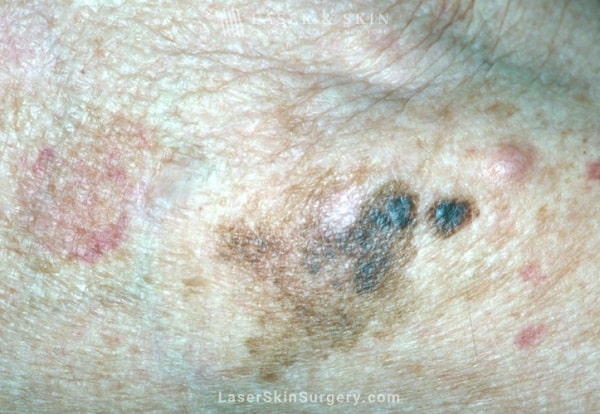
What is Melanoma?
Malignant melanoma develops when the pigment-producing cells in the skin become cancerous.
- Accounts for 5% of cutaneous malignancies but the highest number of deaths
- Incidence of new melanoma diagnoses is increasing annually in the US, but the mortality rate is decreasing
- Roughly half of new diagnoses are detected early while the remaining cases are invasive
- Clinical appearance includes asymmetric, irregularly shaped, multi-colored flat, or elevated growths
- Most melanomas arise from normal skin with only 20% developing from existing moles
- Risk factors are sun exposure, tanning beds (increases risk by 75-80%), genetics, numerous moles (dysplastic nevus syndrome), giant congenital nevus (increases risk by 6-20%)
- Types of melanoma include superficial spreading melanoma (most common type), lentigo maligna melanoma, acral lentiginous melanoma, and nodular melanoma
Learn more about melanoma.
Skin Cancer Treatment Options
Skin Cancer treatment options will vary, depending on the size, type, depth, and location of the lesions. Common treatment options include:
- Topical treatments with agents such as 5-fluorouracil, imiquimod, and ingenol mebutate
- Injectable chemotherapy (cisplatin, methotrexate, 5-fluorouracil)
- Photodynamic therapy – blue or red light with topical 5-aminolevulinic acid
- Cryotherapy – targets the cancerous area with liquid nitrogen, causing it to instantly freeze and eventually sloughs off
- Electrodessication and Curettage – also called electrosurgery, this surgical procedure removes cancerous tissue by cutting it from the skin using a curette (a tool with a circular blade) and using a needle-shaped electrode to treat the area with an electric current to destroy the cancer cells that remain around the wound
- Excision – surgical removal of all the cancerous lesions together with a safe border of surrounding normal skin to prevent the cancer from spreading
- Radiation therapy – uses radiation such as x-rays or electron beams to damage or kill cancer cells
- Immunotherapy – uses medicine to help the body’s immune system find and kill melanoma cells
Mohs Surgery
Mohs surgery removes the cancer with a smaller margin of normal skin with microscopic examination by frozen section technique of all surgical borders during one office visit until the site is cancer-free. Once the site is clear of skin cancer, we address the healing of the wound. Surgical wounds can heal by themselves if relatively small and/or shallow in depth. Deeper or larger wounds are closed in various ways by the MOHs surgeon or, if needed, a plastic surgeon. We have plastic surgeons here in our practice that can consult with our patients when needed. Once healing is complete, we may utilize laser treatments to reduce scarring and improve skin texture, including Pulsed Dye lasers and CO2 lasers, enhancing the treatment’s aesthetic result.

Schedule Your Skin Cancer Screening With A Dermatologist Today
Being proactive about preventing and detecting skin cancer can be lifesaving. While Dr. Bernstein’s webinar is a good place to begin the education process, nothing beats an in-person consultation with a board-certified dermatologist. Contact the Laser & Skin Surgery Center of New York to schedule your consultation at either our Manhattan or Southampton office.
Next, read about…
How to Minimize Stretch Marks After Pregnancy
Homepage // Blog / How to Minimize Stretch Marks After PregnancyPregnancy is a beautiful journey, but it often leaves behind visible reminders on your skin - stretch marks. If you're a new mom looking to address these postpartum changes, you're not alone. While it's...
Revolutionize Your Skin with Micro-coring: The Ultimate Solution for Sagging Skin
Homepage // Blog / Revolutionize Your Skin with Micro-coring: The Ultimate Solution for Sagging SkinAre you troubled by loose, sagging skin and yearning for a tighter, smoother, more youthful complexion? Micro-coring is a revolutionary technique that uses your skin’s...
Laser Skin Tightening: What Is It and How Long Does It Last?
Homepage // Blog / Laser Skin Tightening: What Is It and How Long Does It Last?Laser skin tightening is a cosmetic procedure that uses heat to promote the natural production of collagen and elastin, two proteins that firm and plump skin. With proper care, results can...
By LASER & SKIN SURGERY CENTER OF NEW YORK® | © 2026 All Rights Reserved. | Privacy Policy |The information available on this web site is provided for informational purposes only. This information is not intended to replace a medical consultation where a physician's judgment may advise you about specific disorders, conditions and or treatment options. We hope the information will be useful for you to become more educated about your health care decisions. If you are vision-impaired or have some other impairment covered by the Americans with Disabilities Act or a similar law, and you wish to discuss potential accommodations related to using this website, please contact us at 212.941.5055.
*MDs perform 100% of all medical and cosmetic treatments.